COVID-19 and Planetary Health: How a Pandemic Could Pave the Way for a Green Recovery
Still Only One Earth: Lessons from 50 years of UN sustainable development policy
The COVID-19 pandemic magnifies underlying systemic problems, including ineffective environmental policies, social and economic inequalities, and weak healthcare systems. If we're to truly build back better, policymakers need to promote greater synergies, joint agendas, and linked policies between climate, biodiversity, and health finance. For their part, international organizations and agencies need to break down silos, and take joint action to promote planetary health. (Download PDF) (See all policy briefs) (Subscribe to ENB)
Before the COVID-19 pandemic began in 2020, policymakers already faced sobering health statistics. As noted by the World Health Organization (WHO) and the United Nations Environment Programme (UNEP), nearly 25% of all global deaths are related to economic decisions affecting the environment. Annually, 7 million people die from poor air quality and 3.5 million die from poor water quality. Chemical exposure can cost nearly USD 1 trillion in neurodevelopmental effects in middle and low-income countries. Microplastics, nutrient excess from farm run-off, and zoonotic diseases impact health, well-being, and economic development in overlapping and complicated ways (Myers, 2017).
Existing environmental policies do not effectively support global health and sustainable development objectives. The COVID-19 pandemic has exacerbated these negative trends and has magnified underlying systemic problems, including social and economic inequality and weak healthcare systems. How can sustainable development policies cohesively and proactively address these interrelated challenges to improve human health?

Rethinking the Environment-Health Nexus
The COVID-19 pandemic is the ultimate manifestation of an interconnected world. This zoonotic virus, which jumps pathogenically between wildlife and humans, reminds us of the inter-relatedness of our molecular universe. The swift community lockdown in response to the pandemic reminds us our existence depends on interwoven food and economic pathways. Our neglect of these microscopic and macroscopic interlinkages between human health and the environment is the root cause of the pandemic. Despite decades of scientific warnings, we neglected the ecosystem factors that promote infectious disease transmission.
Human health in the Anthropocene requires an integrated approach. In 2015, the Lancet medical journal in partnership with the Rockefeller Foundation published a landmark report alerting the medical community that humans had damaged the Earth’s natural systems to the point of causing reciprocal risk and damage to human health. The report underlined the urgency and opportunity to address modifiable environmental factors to reduce the global burden of disease and launched an international call for world leaders and experts to support a transdisciplinary approach called “planetary health,” an emerging field that focuses on how human-induced changes in our Earth’s systems impact human health and well-being.
The Effects of Environmental Change and Environmental Degradation on Health
Worldwide, respiratory disease associated with air pollution is rampant. There is a high prevalence of chronic lung inflammation, increased acute asthma, and nasal and sinus allergies, often requiring life-long medication. According to the Lancet Commission on Pollution and Health, respiratory disease can lead to lung cancers and diseases that affect the heart, such as heart attack, stroke, high blood pressure, and high cholesterol. Heart disease has been the leading cause of death globally for two decades and is rising.
Diseases caused by water contamination continue to challenge clinicians, especially among marginalized and low-income populations, in post-disaster settings, and in communities in conflict. Without comprehensive water regulation, antibiotic treatment is a short-term solution to outbreaks of microbial diarrhea that stem from ecosystem disruption in the form of biodiversity loss, excess nutrient run-off from farms, or other human contamination. Viral diseases arising from vectors living in water ecosystems, like mosquitos, also strain health systems. Communities are grappling with increasing incidences of acute and chronic hematological (Malaria), arthritic (Dengue, Chikungunya), or developmental (Zika) disorders. These are exacerbated by climate change, which in turn can bring infected mosquitos to non-endemic and immune system-naive countries.
Climate change is one of the greatest threats to public health (Haines & Ebi, 2019). Rising temperatures, rising sea levels, and extreme weather events pose increasing risks for human well-being (Watts et al., 2019), including injuries, fatalities, mental health impacts, and mass migration (Andrews et al., 2018).
Long-term environmental exposure to and accumulation of toxins, dioxins (persistent organic pollutants), and endocrine disrupting chemicals in our bodies are, or are suspected to be, linked to organ damage, cancer, developmental and neurological disorders, and hormone dysfunction.
Environmental degradation also affects the mental and emotional health and well-being of communities and individuals. Communities may suffer forced displacement, contributing to mental and emotional trauma. These events may additionally trigger psychological illness seeded by underlying, long-standing, environmental injustice, health disparities, and gender inequities. In urban settings, lack of access to green space has also been shown to contribute to poor moods and sleep cycles. It is worth noting the increase in the global prevalence of depression disorders and their correlation with both environmental change and increasing social and economic inequality.
Women and girls’ health and well-being are impacted by environmental degradation and climate change. This is seen in increased stress, higher rates of domestic violence, reduced access to reproductive services and contraception, and reduced access to education and independent livelihoods. Moreover, the disproportionate number of women and girls affected by the COVID-19 pandemic underscores the need to address the links between environment, gender inequality, and poverty.
Food systems are paradoxically a threat to human health. According to the sixth Global Environmental Outlook, the agrifood system is inefficient, environmentally detrimental, and poorly aligned with optimal nutritional needs. Current food system production yields high emission goods, like animal protein and dairy products, and steers dietary habits toward the overconsumption of low nutrition foods, like processed foods and snacks, which are cheaper and more accessible. As a result, both developed and developing countries face a widespread combined burden of poor eating (overeating or under) and micronutrient deficiency. The global incidence of diabetes increased 70% in the last twenty years, and clinics treat numerous obese patients taking multiple chronic medications to regulate their metabolism. The disruption caused by the COVID-19 pandemic led to the closure of markets, decreased production and processing, and restricted food transport including imports, exports, and food assistance. These simultaneous shocks have led to an estimated 80–130 million additional food insecure people.
Loss of biodiversity and ecosystem integrity weakens health systems and changes our exposure to pathogens. At the community level, ecosystem degradation limits the availability of natural medicines and the sustainability of traditional knowledge, as well as opportunities to identify new drugs to treat cancer, viral infections, neurological and brain disorders, and other elusive diseases. Antimicrobial resistance, influenced by unregulated and non-harmonized use of antimicrobial drugs across the veterinary, livestock, and human health sectors, threatens the long-term effectiveness of antimicrobial drugs and the ability to treat bacterial infections and diseases. Studies show biodiversity loss seems to increase emergence and exposure to new strains or new hosts of infectious disease (Myers, 2017).
Deforestation and manufactured waterways (e.g., hydropower and irrigation systems) may increase risk of exposure to more or new harmful microbes. Changes that lead humans to encroach on an ecosystem, such as expanding agricultural land, bushmeat hunting, or legal and illegal wildlife trafficking increase human exposure to zoonotic diseases. This includes coronaviruses (MERS, SARS and COVID-19), HIV and Ebola, monkeypox virus, and avian and swine influenza. The WHO and the Convention on Biological Diversity (2015) highlight the finding over a 68-year period that 60% of emerging infectious diseases are zoonoses and more than 75% of those are from wildlife.
International Recognition of the Environment-Health Nexus
The Stockholm Declaration and Action Plan adopted at the 1972 United Nations Conference on the Human Environment was the first intergovernmental conference outcome to recognize the right to a healthy environment. It further recognized environmental disturbance and destruction as “harmful to the physical, mental and social health of man.” The global conversation highlighted the need for integrated environment and development policies at a number of major events: 1992 Earth Summit, 1994 International Conference on Population and Development, 1995 Fourth World Conference on Women, 2000 UN Millennium Summit, and 2002 World Summit on Sustainable Development. However, practical engagement on the links between environment and health remained siloed.
In 2005, the Millennium Ecosystem Assessment (MA) highlighted environmental degradation as a significant barrier to achieving the Millennium Development Goals (MDGs), specifically addressing and reducing malnutrition, infectious diseases, maternal mortality, exposure to unsafe drinking water, and poverty. In its synthesis on human health, the MA outlined that ecosystems provide a number of services—provisioning, regulating, cultural, and supporting—whose losses would adversely affect human health. The MA recommended building capacity for low-income communities to adapt to environmental change. This would prevent a downward health spiral where environmental degradation begets poverty that generates further environmental degradation.
Ecosystem services are indispensable to the well-being and health of people everywhere.
The current development paradigm—the 2030 Agenda for Sustainable Development and its Sustainable Development Goals (SDGs)—takes a step away from silos and towards synergistic work, in part by providing interdisciplinary metrics to guide assessment and action. Trends in global engagement have followed suit, as seen in the collaborations between environmental fora, like the UN Framework Convention on Climate Change (UNFCCC), Intergovernmental Panel on Climate Change (IPCC), Convention on Biological Diversity (CBD), and the Intergovernmental Platform on Biodiversity and Ecosystem Services (IPBES), among others, and in resolutions adopted by the World Health Assembly (WHA) on environmental issues, including on climate, air pollution, and antimicrobial resistance.
COVID-19 and Planetary Health: Mainstreaming and Mobilizing Green Recovery
Major international actors and agencies see planetary health as a “cross-cutting solution” (Figure 1) to achieve the SDGs and deliver on the 2030 Agenda (UNEP, 2016; UNEP, 2019).
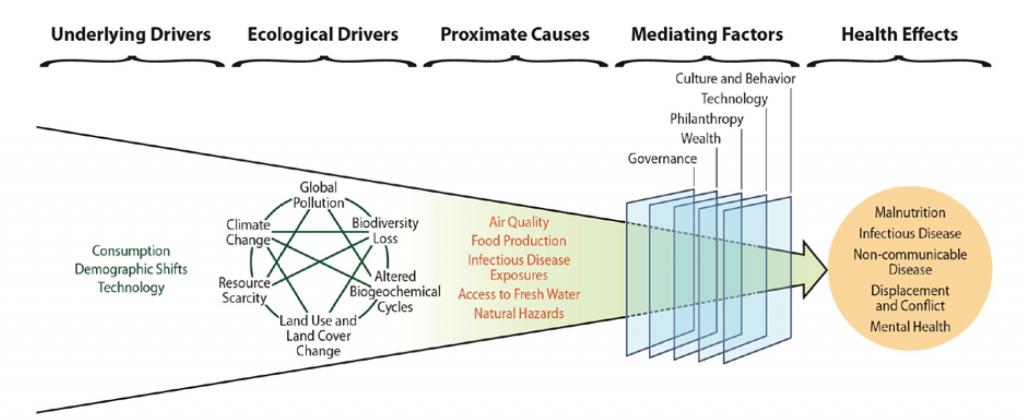
The COVID-19 pandemic presents an opportunity to reconsider how we structure and integrate our food, waste, water, and energy systems. It also means thinking about long-term health and well-being by evaluating co-benefits across environmental, social, and economic domains.
Innovative financing, built on cost-benefit analyses comparing health savings to the costs of mitigating environmental change and damage, is fundamental to this new paradigm (Myers, 2017; UNEP, 2019). For instance, IPBES estimates the annual cost of zoonotic disease is in excess of USD 1 trillion, far higher than the USD 78-91 billion the Organisation for Economic Cooperation and Development (OECD) estimates for annual global biodiversity finance. Preventative actions, such as disease monitoring, retained forest cover, reductions in interspecies transmissions, and regulation of the wild meat trade, are estimated at USD 22-31 billion annually. This is significantly less than the mortality and economic costs of a pandemic like COVID-19, which is estimated at more than USD 8 trillion (Dobson et al., 2020). Similarly, health savings from policies that reduce air pollution are projected to be even greater, USD 23 trillion over the long term (UNEP, 2019). These data are compelling and warrant deeper examination, replication, and standardization across sectors.
Socio-ecological determinants of zoonotic disease spread:
- Land-use change
- Human susceptibility to infection
- Agricultural industry change
- International travel and commerce
- War and famine
- Medical industry change
- Climate and weather
- Demography and behaviour
- Bushmeat
- Breakdown of public health
- Food industry changes
(Loh et al., 2015)
COVID-19 resource mobilization can steer green recovery not only to “build back better” but to take up long-held environmental sustainability and health evidence to effectively safeguard against future pandemics and other global challenges. This view should fully address climate change and the energy economy, the waste cycle, and food systems, with emphasis on ecosystems, biodiversity, and social inclusion and equality. It should also drive transformation in data collection, integration of sectors, and modes of engagement between international actors. Key priority areas are as follows.
Strengthen climate resilience in our economies and ecosystems and promote convergence between climate, biodiversity, and health finance. Sustainable development finance must include health co-benefits. Only 0.5% of multilateral climate finance is earmarked specifically for health projects (WHO, 2018a). The WHO (2018b) notes several specific barriers that present opportunities for enhanced integration of health and climate policy, including:
- Only 10% of nationally determined contributions funded by the Green Climate Fund include health-related activities
- The majority of national adaptation plans do not include health or specifically analyze the burden of climate-sensitive disease or prioritize health actions.
- Health actors are not well connected to international climate change processes.
- There is little formal engagement between the health and transportation sectors and health and energy sectors.
Move towards a resource-efficient circular economy and ecosystem-based approach. Waste, in all its forms, is a serious health hazard and leads to disease. Policymakers need to promote ambitious policies to reduce air, land, soil, fresh water, and ocean pollution. An emphasis on strengthening global coordination on marine litter and microplastics and support for the Strategic Approach to International Chemicals Management (SAICM) to adopt ambitious post-2020 recommendations are needed. Supply chains should focus on the life-cycle approach and not rely on environmentally harmful subsidies and other perverse incentives.
Steer food systems toward sustainability and improved food and nutritional security. Under a business-as-usual scenario, the way we produce and consume food increases risks related to climate change, water insecurity, and malnutrition (CFS, 2021). Governments should support diversification in food system production while also redirecting consumer food patterns, including promoting domestic food production and local food culture and knowledge. Linking environment and health goals should reduce reliance on high emission foods, assess both nutritional value and sustainability of consumption patterns, and connect national nutritional dietary guidelines to sustainability objectives (UNEP, 2019).

Support and fund biodiversity and ecosystem protection to prevent outbreaks of infectious diseases and strengthen nutritional security. Policymakers should increase and improve sustainable land and forest management to maintain genetic diversity and significantly reduce habitat loss, unsustainable land-use change, deforestation, and fragmentation. To prevent outbreaks of infectious disease, policy measures should promote conservation that reduces the transmission of pathogens, and strengthens the resilience of human immune systems, such as through controls on antimicrobial use and biocides. Biodiversity action plans and impact assessments should include health metrics and adopt the One Health approach to monitoring. Both the CBD and the WHO call for improved and integrated metrics to evaluate and monitor national biodiversity and health data.
Reconfigure data metrics at all scales to include interdisciplinary and overlapping risk factors. Policymakers should draw on databases like the Global Burden of Disease study that provides ongoing analyses of both health and environmental risk factors since 1990. Policymakers should compare effects of different and combined risk factors, such as nutrition and zoonotic disease, on health and use these in cost-benefit analyses.
Promote broad multi-sectoral and transdisciplinary integration. Environment and health ministries need to work together and link policy and programming at all scales. Finance ministers should work with medical leaders to design economic recovery packages that balance economic growth with human well-being and the environment (WHO, 2020). Medical professionals should be encouraged to engage in environment and sustainable development planning and policymaking. Health curricula should incorporate environmental and sustainable development issues. Researchers must engage in transdisciplinary approaches, incorporating, for example, traditional knowledge.
International organizations and agencies need to break down silos, take joint action, and integrate policy and programming within and among other multilateral organizations to promote planetary health. The 2030 Agenda provides a global blueprint for increased collaboration between international organizations, national and sub-national governments, civil society, the private sector, and other relevant stakeholders to ensure long-term policies are supportive of planetary health. Environmental mandates must include health factors and global health actors must realize their role in the environmental community. The importance of gender equity and environmental justice must be recognized and brought to the forefront of discussion.
Decisions made in the coming months can either ‘lock in’ economic development patterns that will do permanent and escalating damage to the ecological systems that sustain all human health and livelihoods, or, if wisely taken, can promote a healthier, fairer, and greener world.
Overcoming Multidimensional Crises and Safeguarding against Future Pandemics
COVID-19 has uncovered the gaps of existing, fragmented policies and systems, and has made it impossible to ignore the potential repercussions of future health and environmental decisions. At the same time, it has created a platform for comprehensive social, economic, and environmental change. Sustainable and equitable development requires integrated approaches. Effective policies must be cross-cutting and intersectional rather than isolated actions or singular technological improvements. Implementing green recovery approaches will create multiplier effects, including on health, gender and social equity, and economics.
COVID-19 can be an opportunity to use planetary health as a new guiding development narrative. Health and environment should be considered as one and become eligible for joint funding opportunities. Examples of funders championing this recommendation include the Wellcome Trust and the Gordon and Betty Moore Foundation. More than the exception, synergies between environmental and health policies must be the rule.
Works Consulted
Andrews, O., Le Quéré, C., Kjellstrom, T., Lemke, B., & Haines, A. (2018). Implications for workability and survivability in populations exposed to extreme heat under climate change: A modelling study. The Lancet Planetary Health, 2(12), e540–e547. https://doi.org/10.1016/s2542-5196(18)30240-7
Committee on World Food Security (CFS). (2020). Impacts of COVID-19 on food security and nutrition: Developing effective policy responses to address the hunger and malnutrition pandemic. CFS High-Level Panel of Experts on Food Security and Nutrition Issues Paper. Food and Agriculture Organization of the UN. http://www.fao.org/3/cb1000en/cb1000en.pdf
CFS. (2021). CFS Voluntary Guidelines on Food Systems and Nutrition. Food and Agriculture Organization of the UN. http://www.fao.org/fileadmin/templates/cfs/Docs1920/Nutrition_Food_System/Negotiations/NE_982_47_8_VGFSYN.pdf
de Paula, N. & Mar, K.A. (2020). Moving as One. Integrating the Health and Climate Agendas for Planetary Health in a Post-Pandemic World. IASS Policy Brief, 2/2020. https://doi.org/10.2312/iass.2020.025
Dobson, A., Pimm, S., Hannah, L., Kaufman, L., Ahumada, J., Ando, A., . . . Vale, M. (2020, July 24). Ecology and economics for pandemic prevention. Science 369 (6502): 379-381. https://science.sciencemag.org/content/369/6502/379
Haines, A. & Ebi. K. (2019). The Imperative for Climate Action to Protect Health, The New England Journal of Medicine, 380: 263-273 https://www.nejm.org/doi/full/10.1056/nejmra1807873
Loh, E. H., Zambrana-Torrelio, C., Olival, K. J., Bogich, T. L., Johnson, C. K., Mazet, J. A. K., Karesh, W., & Daszak, P. (2015). Targeting transmission pathways for emerging zoonotic disease surveillance and control. Vector-Borne and Zoonotic Diseases, 15(7): 432–437. https://doi.org/10.1089/vbz.2013.1563
Myers, S. (2017). Planetary health: Protecting human health on a rapidly changing planet. The Lancet. 390 (10114): 2860-2868. https://doi.org/10.1016/S0140-6736(17)32846-5
Myers. S. (2020). An Introduction to Planetary Health. In Planetary Health: Protecting Nature to Protect Ourselves. Island Press.
UNEP. (2016). Healthy environment, healthy people. https://wedocs.unep.org/bitstream/handle/20.500.11822/17602/K1602727%20INF%205%20Eng.pdf
UNEP. (2019). Global Environment Outlook – GEO-6: Healthy planet, healthy people. United Nations Environment Programme. https://wedocs.unep.org/handle/20.500.11822/27539
Watts, N., Amann, M., Arnell, N., Ayeb-Karlsson, S., Belesova, K., Boykoff, M., Byass, P., Cai, W., Campbell-Lendrum, D., Capstick, S., Chambers, J., Dalin, C., Daly, M., Dasandi, N., Davies, M., Drummond, P., Dubrow, R., Ebi, K. L., Eckelman, M., … Montgomery, H. (2019). The 2019 report of The Lancet Countdown on health and climate change: ensuring that the health of a child born today is not defined by a changing climate. The Lancet, 394(10211): 1836–1878. https://doi.org/10.1016/s0140-6736(19)32596-6
World Health Assembly. (2018). Report of the Director-General: Health, environment and climate change - Human health and biodiversity (A71.11). 71st World Health Assembly. https://apps.who.int/gb/ebwha/pdf_files/WHA71/A71_11-en.pdf
WHO. (2018a). UNFCCC COP24 Special Report: Health & climate change. World Health Organization https://apps.who.int/iris/bitstream/handle/10665/276405/9789241514972-eng.pdf
WHO. (2018b). The 1.5 health report: Synthesis on health & climate science In the IPCC SR1.5. WHO/CED/PHE/EPE/19.11. https://www.who.int/publications/i/item/the-1.5-health-report
WHO. (2020). Manifesto for a healthy recovery from COVID-19: Prescriptions for a healthy and green recovery from COVID-19. World Health Organization. https://www.who.int/docs/default-source/climate-change/who-manifesto-for-a-healthy-and-green-post-covid-recovery.pdf
WHO and CBD. (2015). Connecting global priorities: Biodiversity and human health: A state of knowledge review. http://apps.who.int/iris/bitstream/10665/174012/1/9789241508 537_eng.pdf
You might also be interested in
Web of resilience
Pakistan's development model has still not recognised the limits of the natural environment and the damage it would cause, if violated, to the sustainability of development and to the health and well-being of its population. Pakistan’s environment journey began with Stockholm Declaration in 1972. A delegation led by Nusrat Bhutto represented the country at the Stockholm meeting, resulting in the establishment of the Urban Affairs Division (UAD), the precursor of today’s Ministry of Climate Change. In setting the country’s environmental agenda, we were inspired by the Stockholm Principles, but in reality, we have mostly ignored them for the last five decades.
Rethinking Investment Treaties
International investment treaties and their investor–state dispute settlement (ISDS) system are facing growing scrutiny. But what would an alternative system—one fit for the challenges of the 21st century—look like?
The Legacies of the Stockholm Conference
Fifty years after Stockholm, we face a triple planetary crisis of climate change, nature and biodiversity loss, and pollution.
Coral Reefs: Strategies for Ecosystems on the Edge
Local stressors and climate change are causing a sharp decline in coral reefs. A loss of 70–90% of warm-water reefs could occur by 2050.



